Can I Still Run After Knee Replacement Surgery?

(Photo: Getty Images)
When ultramarathoner Richard Donovan came to Kevin R. Stone, MD, of The Stone Clinic in San Francisco, he’d already been told by other doctors that he needed total knee replacements – and that he’d never run again.
Fortunately, Stone – a pioneer of advanced orthopedic surgical and rehabilitation techniques to repair, regenerate, and replace damaged cartilage and ligaments – took a different approach, performing two partial knee replacements in 2019 and 2021. And Donovan, who is in his 50s, didn’t just keep running. In 2022, after running the Boston Marathon, he completed a three-month, 3200-mile run across America, logging over 40 miles a day.
Donovan’s initial experience of being told he’d have to stop running is not uncommon, as many of us with knee problems can attest. And while Donovan’s status as an elite athlete certainly provided an additional level of motivation to find a solution that kept him running, there are a lot of people out there who are sitting out from their sports unnecessarily.

Knee Replacement Surgery: Understanding Your Options
“Eighty percent of people who are told they need a total knee replacement don’t [need one],” Stone said – and that’s for a few reasons.
For one thing, knees don’t usually wear out all over the place; it’s typically on one side or the other, he said. There are many stages of arthritis before a complete wearing down of the articular cartilage, and, if they’re not yet to the bone-on-bone stage, there’s the possibility of a biologic knee replacement, which means they can regrow that articular cartilage and replace their meniscus cartilage.
Even for the folks who have reached that bone-on-bone stage, they may be eligible for a partial knee replacement, where only the worn-out part of the knee is replaced, said Stone. “That was the case in Richard Donovan,” he explained.
Of course, some people truly do have tri-compartmental arthritis, which means that all parts of the knee are arthritic. But even in this case, Stone has good news – and it involves robots.
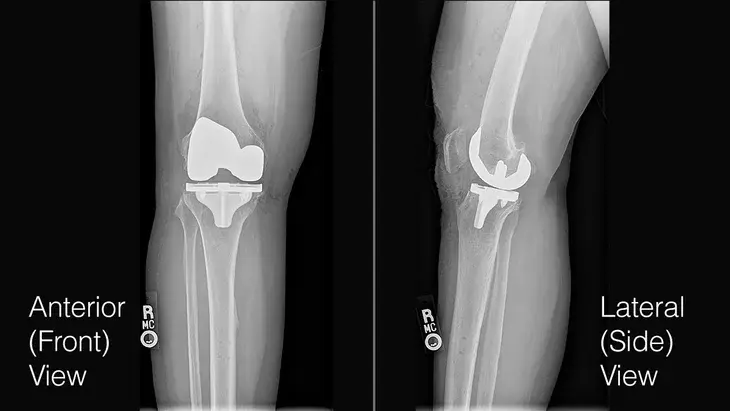
“Those people can have a new form of a knee replacement, which is really a knee resurfacing where we use a robot to precisely remove the arthritic part of the joint and cap it with a metal cap on the end of the femur, and a metal and plastic tray on the tibia,” he said. That robotic precision is so good that cement is not needed, Stone explained. They press fit the new component right onto the bone, and the body will grow into the porous undersurface of the component.
RELATED: Runner’s Knee? Tight Hip Flexors? Learn how to prevent common upper leg injuries.
“What this means for all the runners of the world who’ve been told they can’t run again, they often can,” he explained, “if, number one, they have a biologic replacement; or number two, they have a partial replacement that’s done with robotic accuracy; or number three, they have a total replacement done with robotic accuracy and is uncemented.”
Stone’s commitment to finding ways to keep patients active is no surprise; the man wrote a book called Play Forever, and he takes that motto to heart. “Our goal is to help you drop dead at 100 playing the sport you love, so let’s pull out every resource to help you do that,” he said.
After all, he said, if you tell an active person to stop running and exercising due to poor knee health or a joint replacement, chances are that they’ll become depressed, lose muscle, and lose bone mass. On the other hand, if you encourage a patient to increase their exercise, they build bone, build muscle, and stay happy. That attitude change, along with the changes with precision surgery and the new biologic options, have created a whole new world for shoddy-kneed athletes.
Talking to Your Doctor About Knee Replacement Surgery
If you’re experiencing knee pain, now is the time to take action. “There’s no reason to live in pain,” he said. “Life is short, and your opportunities to exercise without pain are precious. There’s no reason to give them up.”
However, it’s important to note that although the techniques Stone mentioned are taught and used worldwide, not all doctors take the same approach to getting patients back to their activities. Stone recommends asking about your doctor’s outcomes and experience to make sure you’re on the same page. “If they only do total knee replacements, they’re probably not going to talk to a patient about the other options,” he said. If you discover that you and your doctor don’t share the same goals, that’s a sign that you may want to get a second (or third) opinion.
“The other thing a patient should know is that we’re in what I call the anabolic era of sports medicine,” Stone explained. “That means we can do injections, and we have techniques for tissue regeneration.” You might be familiar with some of these techniques, like PRP (platelet-rich plasma – aka growth factors from the patient’s own platelets) paired with hyaluronic acid (HA) or factors that recruit the body’s own stem cells and their progeny to the site of injury, and Stone said this field is exploding – in a good way. “For many patients who have arthritic joints, just this combination of PRP and HA is a great rehab program,” he said. “They come in for their once or twice a year ‘lube job’ as they call it, and it can relieve their symptoms for quite a while.” This is not a cure, to be clear, but it does keep them out of his operating room and in their sport.
Success isn’t only achieved via surgery or injection, though. The post-op or post-treatment approach also plays a crucial role, and Stone aims to have all his patients begin rehab the very next day. “The most important aspect of that is that we try to help our patients see themselves as athletes in training, not as patients in rehab,” he said. He encourages them to have a mindset that they’re starting their training to get back to their event, starting on Day 1. “Wondering when you can get back to your training is the wrong approach, I’d argue,” he said.
At his clinic, patients take sport tests to help their surgeon, physical therapy team, and rehab team better coordinate their return to performance. If a patient’s goal is to simply walk without pain, they’ll set a training program around balance and gait to help them achieve that. “And, if your goal is to come back to an Ironman, then let’s be sure you can pass all of our fitness tests to come back safely,” he said. “Let’s set the program with the goal of helping you come back better than you were before.”